Imagine your body’s defense system is like a security team. Usually, they keep an eye on the perimeter, letting friends in and stopping intruders. But with immune checkpoint inhibitors (ICIs), the boss gives that team a megaphone and orders them to attack everything that looks suspicious. This powerful boost helps destroy cancer cells, but it doesn’t always tell the difference between a tumor and healthy tissue. The result? Immune-related adverse events (irAEs). These are not just typical chemotherapy side effects; they are inflammatory or autoimmune reactions triggered by the drug itself. You might be thinking, "Is this dangerous?" It can be, if ignored. But here is the good news: we know how to handle them. With proper recognition and treatment, most patients stay on track with their cancer care. Let’s break down what you need to watch for, how doctors grade these events, and why acting fast matters more than ever.
What Exactly Are irAEs?
Unlike traditional chemo, which kills fast-growing cells indiscriminately, ICIs work by removing the "brakes" from your T-cells. This allows your immune system to recognize and attack cancer. However, when those brakes come off, the immune system can go into overdrive. It starts attacking normal organs-your skin, gut, lungs, or thyroid.
This phenomenon was first systematically recognized after the FDA approved ipilimumab in 2011 for metastatic melanoma. Since then, we’ve seen these drugs become standard for lung, kidney, bladder, and many other cancers. A large meta-analysis published in PMC in 2021 showed that about 83% of patients on CTLA-4 inhibitors experience some form of irAE. For PD-1 inhibitors, that number drops to around 72%, and for PD-L1 inhibitors, it’s roughly 60%. While those percentages sound high, remember that many of these events are mild and manageable.
The key takeaway? irAEs are expected, not accidental. They signal that the drug is working, but they require careful monitoring because they can affect virtually any organ system.
Recognizing the Signs: Which Organs Are at Risk?
You don’t need to memorize every possible symptom, but knowing the common patterns helps you catch issues early. irAEs often appear within the first three months of treatment, though they can show up later or even after you stop the drug. Here are the most frequent culprits:
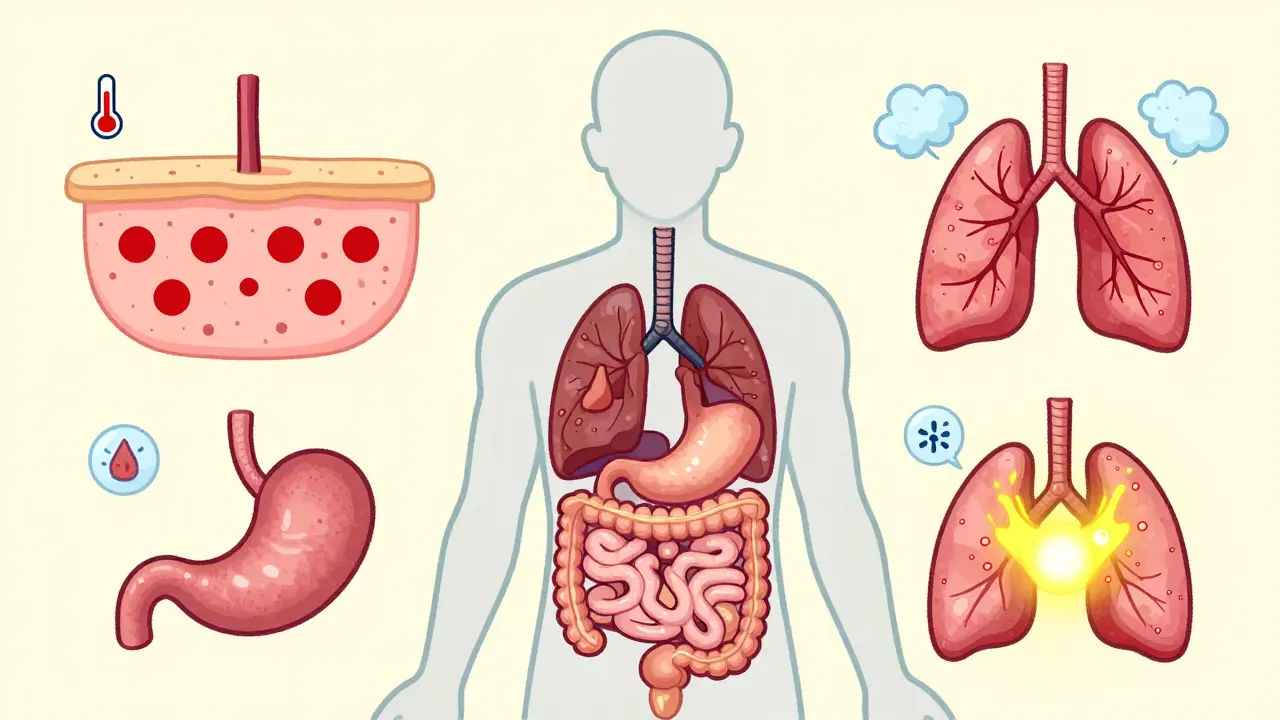
- Skin (Dermatologic): This is the most common site. You might see a rash, itching, or psoriasis-like patches. It usually looks like a sunburn or eczema flare-up.
- Gut (Gastrointestinal): Diarrhea is the big red flag here. If you have more than four bowel movements a day compared to your baseline, or if there is blood in your stool, call your doctor immediately. This could be colitis.
- Lungs (Pulmonary): Pneumonitis presents as shortness of breath, dry cough, or chest pain. It can develop quickly, so don’t wait for a scheduled appointment if you feel winded.
- Endocrine System: Thyroid dysfunction or hypophysitis (pituitary inflammation) might not cause obvious pain. Instead, look for fatigue, unexplained weight changes, headaches, or vision changes. These often require hormone replacement rather than immunosuppression.
- Liver (Hepatitis): This one is tricky because it rarely hurts. Doctors rely on blood tests to check liver enzymes. Elevated bilirubin or AST/ALT levels are the warning signs.
Rare but serious events include myocarditis (heart inflammation) and neurotoxicity. Myocarditis has a higher mortality rate, so symptoms like palpitations, extreme fatigue, or swelling in the legs need urgent evaluation.
Grading the Severity: The CTCAE System
Not all irAEs are created equal. To decide on treatment, oncologists use the Common Terminology Criteria for Adverse Events (CTCAE) system. This standardized scale grades toxicity from 1 to 5. Understanding your grade helps you understand the urgency.
| Grade | Severity | Typical Action |
|---|---|---|
| 1 | Mild | Continue immunotherapy; monitor closely. |
| 2 | Moderate | Hold immunotherapy; start oral steroids. |
| 3 | Severe | Stop immunotherapy; hospital admission likely; IV steroids. |
| 4 | Life-threatening | Permanent discontinuation; intensive care support. |
For example, Grade 1 diarrhea means you have fewer than four extra stools per day. Grade 3 means you have seven or more, or you can’t eat or drink due to symptoms. The grade dictates whether you stay home or head to the ER.
Treatment Protocols: Steroids and Beyond
The cornerstone of treating irAEs is corticosteroid therapy. Think of steroids as the "off switch" for your overactive immune system. The type and dose depend entirely on the grade.
For Grade 2 events, doctors typically prescribe oral prednisolone at 1 mg/kg/day. You’ll hold your immunotherapy until symptoms drop back to Grade 1. For Grade 3 or 4 events, the approach is aggressive. You may receive intravenous methylprednisolone (1-2 mg/kg/day, up to 1 gram daily) for the first few days, followed by high-dose oral steroids.
Here is where patience pays off. You cannot just stop steroids abruptly. The Steroid Tapering Protocol requires gradually reducing the dose over 4 to 6 weeks. Stopping too fast can cause rebound symptoms, making the irAE worse. A study in the ASCO Journal of Clinical Oncology emphasizes that this slow taper is critical for long-term resolution.
What if steroids don’t work? About 10-15% of cases are "steroid-refractory," meaning no improvement after 48 hours. In these scenarios, doctors add other immunosuppressants:
- Infliximab: Often used for colitis (gut inflammation). It targets TNF-alpha, a key inflammatory protein.
- Mycophenolate mofetil: Another option for refractory cases.
- IVIG (Intravenous Immune Globulin): Used for neurological or severe systemic issues.
- Cyclophosphamide: Reserved for very severe, life-threatening cases.
A 2024 update from the Society for Immunotherapy of Cancer (SITC) also highlights vedolizumab as an effective alternative for steroid-refractory colitis, showing better response rates in recent trials.
Does Treating irAEs Ruin Cancer Control?
This is the question that keeps many patients awake at night. "If I suppress my immune system to treat the side effect, won’t the cancer come back?" Early theories suggested yes, but current data says no.
Multiple studies, including reviews in Cancer Therapy Advisor and JAMA Oncology, show that using immunosuppressants for irAEs does not negatively impact tumor response. In fact, managing irAEs effectively allows you to continue or restart immunotherapy sooner, maintaining control over the cancer. The goal is balance: calm the storm without shutting down the entire defense system permanently.

The Human Side: Quality of Life and Support
Managing irAEs isn’t just about medical charts. It’s about living through the process. A survey on ASCO’s My Oncofertility platform revealed that 68% of patients struggled with the quality-of-life impacts of steroid treatment. Common complaints included insomnia (72%), weight gain (65%), and mood swings (58%).
If you’re experiencing these, talk to your care team. There are supportive measures available:
- Sleep hygiene: Take steroids in the morning to minimize insomnia.
- Diet adjustments: Low-sodium diets help with fluid retention and weight gain.
- Mental health support: Mood disturbances are real side effects of both the disease and the treatment. Counseling or medication can help.
Oncology nurses report that patient education is a huge gap. Many people don’t realize that reporting a mild rash or loose stool early can prevent a hospital stay. Don’t wait. If something feels "off," say something. Early intervention reduces hospitalization rates significantly, according to real-world evidence from Flatiron Health.
When to Call the Doctor
You don’t need to be a diagnostician, but you do need to be vigilant. Contact your oncology team immediately if you experience:
- Persistent diarrhea (more than 4 stools/day above baseline).
- New or worsening shortness of breath or cough.
- Severe headache, vision changes, or confusion.
- Yellowing of the skin or eyes (jaundice).
- Chest pain or irregular heartbeat.
Remember, your care team expects these calls. It’s part of the job. Having a clear plan and knowing who to call can make the difference between a minor inconvenience and a major crisis.
Looking Ahead: Better Management in 2026
We are getting better at predicting and preventing irAEs. Recent research in Nature Medicine identified baseline serum IL-17 levels as a potential biomarker for severe irAEs. While not yet routine, this suggests a future where we might tailor immunotherapy doses based on individual risk profiles.
Additionally, institutions like MD Anderson have dedicated "immune toxicity teams" that improve protocol adherence and reduce complications. As combination therapies increase-with hundreds of trials testing new ICI pairings-specialized clinics will become even more common. The European Society for Medical Oncology (ESMO) is also pushing for standardized patient education materials to ensure everyone understands their risks.
The landscape is changing, but the core message remains: awareness saves lives. By recognizing the signs and trusting the treatment protocols, you empower yourself to navigate this complex therapy safely.
How long do irAEs last?
Most irAEs resolve within 4 to 8 weeks with appropriate treatment. However, about 10-15% of cases become chronic, requiring lifelong management such as hormone replacement for endocrine issues or sustained low-dose immunosuppression.
Can I get irAEs after stopping immunotherapy?
Yes. Although most occur during treatment, irAEs can develop months after discontinuing the drug. This is why ongoing monitoring is essential, even after you finish your course of therapy.
Are irAEs different from regular chemo side effects?
Absolutely. Chemo side effects are usually due to cell death and toxicity (like nausea or hair loss). irAEs are inflammatory or autoimmune reactions caused by an overactive immune system attacking healthy organs. They require different treatments, primarily steroids.
What should I do if I have mild diarrhea?
Monitor your symptoms closely. If you have more than four additional bowel movements per day compared to your normal baseline, contact your doctor. Do not take anti-diarrheal medications without consulting your oncology team, as they can mask symptoms of severe colitis.
Do steroids weaken my ability to fight cancer?
Current evidence shows that short-term steroid use for irAEs does not negatively impact tumor response. Managing the side effect allows you to continue or resume immunotherapy, which is crucial for controlling the cancer.
