What Is Guillain-Barré Syndrome?
Guillain-Barré Syndrome is a rare autoimmune disorder where the body’s immune system mistakenly attacks the peripheral nerves. It was first identified in 1916 by three French doctors-Guillain, Barré, and Strohl-and has been studied extensively since. The condition affects about 1 to 2 people per 100,000 each year in the U.S., with roughly 3,000 to 6,000 cases annually. Symptoms usually start with tingling or weakness in the legs and spread upward, often reaching the arms and face. In severe cases, it can paralyze muscles used for breathing, making it a medical emergency.
Most people develop GBS after an infection. The most common trigger is Campylobacter jejuni, a bacteria linked to food poisoning, which is involved in 20% to 40% of cases. Other triggers include cytomegalovirus, Epstein-Barr virus, Zika virus, and, rarely, vaccines or surgery. The immune system gets confused, targets nerve coverings called myelin, and disrupts signals between the brain and muscles.
How Does GBS Progress?
Weakness in GBS doesn’t come on slowly. It typically starts in the feet and legs, then moves up the body over days or weeks. About 85% to 90% of patients experience this ascending pattern. Within 21 days, most reach their worst point. Half of those affected develop facial weakness, trouble swallowing, or double vision due to cranial nerve involvement. Reflexes, like the knee-jerk reaction, disappear completely in almost all cases.
The most common subtype in North America and Europe is Acute Inflammatory Demyelinating Polyradiculoneuropathy (AIDP), which makes up 90% of cases. It’s diagnosed using nerve conduction tests that show slowed signals due to damaged myelin. A less common form, called axonal GBS, directly attacks the nerve fibers themselves and tends to be more severe. Both forms can lead to respiratory failure-about 20% to 30% of patients end up on ventilators.
Why IVIG Is the First-Line Treatment
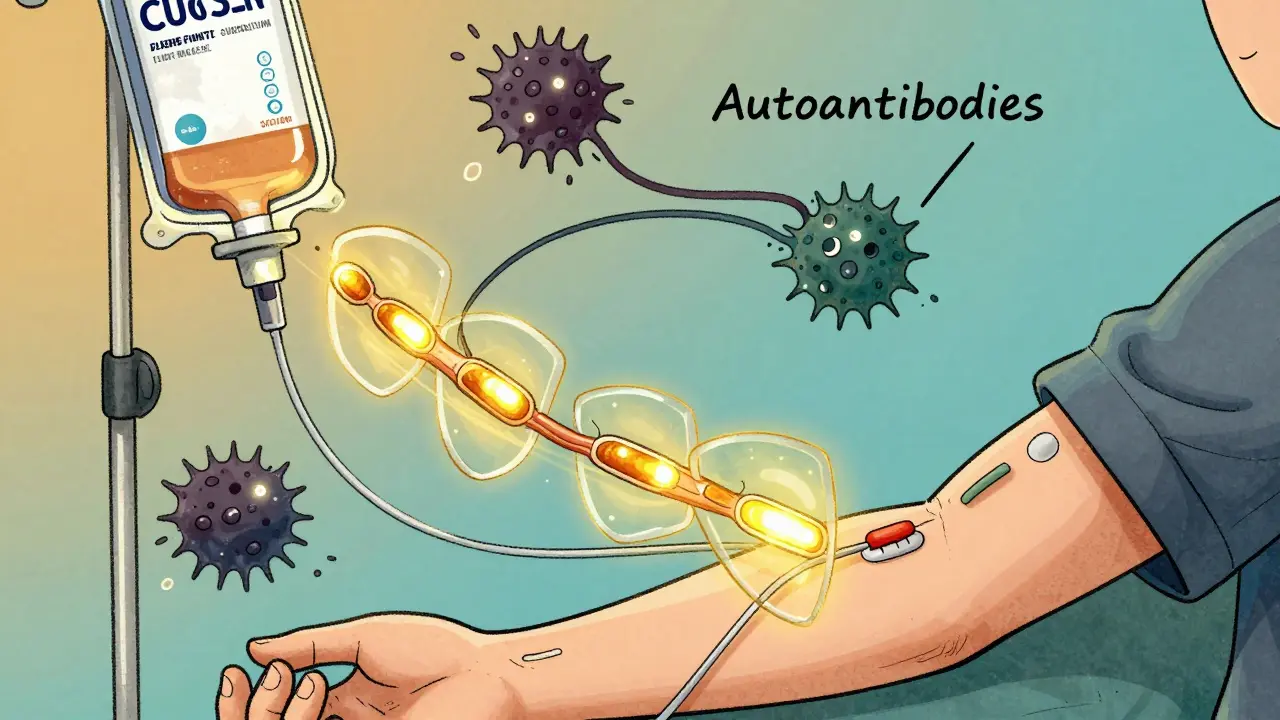
Two treatments are proven to speed recovery: intravenous immunoglobulin (IVIG) and plasma exchange. But IVIG is now the standard in most hospitals. It works by flooding the bloodstream with healthy antibodies from donors, which helps block the harmful ones attacking the nerves.
IVIG is given as a daily infusion for five days straight. The dose is 0.4 grams per kilogram of body weight each day. That means a 70-kilogram person gets about 28 grams per day. Studies show starting IVIG within two weeks of symptom onset cuts recovery time by nearly half. People who get IVIG walk independently about three weeks faster than those who don’t. By four weeks, 60% of treated patients show clear improvement, compared to only 40% without treatment.
One major reason IVIG is preferred over plasma exchange is simplicity. IVIG just needs a regular IV line in the arm. Plasma exchange requires a large central line in the chest or neck, which increases infection risk and is harder to manage. A 2019 study in JAMA Neurology found both treatments worked equally well at four weeks, but patients rated IVIG higher for comfort and ease.
How Effective Is IVIG? Real Numbers
Large clinical trials back up IVIG’s effectiveness. The landmark 1997 trial, known as the Plasma Exchange/Sandoglobulin study, proved both IVIG and plasma exchange were far better than just supportive care. Since then, multiple reviews by the Cochrane Collaboration have confirmed these findings. On average, IVIG reduces the time spent in the hospital by 10 to 14 days.
But it’s not magic. About 20% of people still have lasting weakness after a year. Some struggle with fatigue, numbness, or pain long after the acute phase. Data from the GBS/CIDP Foundation shows:
- 60% recover fully within 6 to 12 months
- 30% have some lasting weakness or need assistive devices
- 10% remain severely disabled
Early treatment matters. Experts like Dr. Michael Levin from the National Institute of Neurological Disorders and Stroke say each day’s delay in starting IVIG reduces its effectiveness by about 5%. That’s why doctors push for hospital admission and treatment within 7 to 14 days-ideally sooner.
Side Effects and Risks of IVIG
IVIG is generally safe, but it’s not risk-free. Common side effects include headaches (25% of patients), fever (15%), and nausea. Some people feel flu-like symptoms during or right after the infusion. A 2022 analysis of online patient forums found 22% of users reported severe headaches during treatment-some described it like a vice crushing their skull.
More serious risks include kidney problems and blood clots. About 1% to 3% of patients develop thromboembolic events, especially those with pre-existing conditions like high blood pressure or dehydration. Patients with IgA deficiency can have life-threatening allergic reactions to IVIG because it contains trace amounts of IgA. That’s why doctors screen for this before treatment.
One rare but devastating complication is acute kidney injury. A patient story on PatientsLikeMe described how her son developed renal failure after the third IVIG dose and needed dialysis for two weeks. While this happens in less than 0.5% of cases, it’s a serious enough risk that doctors monitor kidney function during and after treatment.
Why Not Plasma Exchange or Steroids?
Plasma exchange, or plasmapheresis, removes the patient’s blood plasma-where the harmful antibodies float-and replaces it with donor fluid. It’s effective and works just as well as IVIG in trials. But it’s more invasive. It requires a central line, takes longer, and carries a 30% complication rate compared to 15% for IVIG. It’s often used in emergencies, like when someone is rapidly deteriorating and needs faster action, or if IVIG isn’t available.
Corticosteroids, like prednisone, were once thought to help. But multiple large trials, including a 2017 Cochrane meta-analysis, found no benefit. Steroids didn’t shorten recovery time or improve outcomes. They’re not recommended for GBS anymore.
What Happens in the Hospital?
If GBS is suspected, the patient is admitted immediately. Doctors perform a spinal tap to check for albuminocytological dissociation-a telltale sign where protein levels are high but cell counts are normal. Nerve conduction studies are done within 72 hours. Autonomic instability is common: blood pressure can swing wildly, heart rate can spike or drop. Continuous monitoring is essential.
Respiratory failure is the biggest danger. About 30% of patients need mechanical ventilation within a week. Doctors watch breathing patterns closely and may intubate before the patient is in full crisis. Recovery can take months. Physical therapy starts early, even if the patient is on a ventilator. Many need months of rehab before walking again.
Cost and Access Issues
IVIG treatment costs between $15,000 and $25,000 per course in the U.S. Plasma exchange runs $20,000 to $30,000. While IVIG is cheaper and easier, supply shortages have happened. During the 2020-2022 pandemic, 40% of hospitals reported shortages. Global demand for immunoglobulins has risen, and production is slow-plasma donation and processing take months.
Two brands dominate the U.S. market: Gammagard (Takeda) and Privigen (CSL Behring). Insurance usually covers IVIG for GBS, but prior authorization is often needed. In countries without universal healthcare, cost can delay treatment, which worsens outcomes.
What’s Next for GBS Treatment?
Research is moving toward targeted therapies. Scientists have identified specific antibodies in 65% of axonal GBS cases that attack nerve proteins. This could lead to tests that predict who responds best to IVIG. A 2022 phase 2 trial of eculizumab, a drug that blocks part of the immune system, showed 30% faster recovery. It’s not approved yet, but it’s a promising direction.
The International GBS Outcome Study (IGOS), running since 2022, is tracking 1,500 patients across 30 countries. Early data suggests starting IVIG within 72 hours-instead of 7 days-could improve six-month outcomes by 15%. That’s why hospitals are now pushing for faster diagnosis and treatment.
Recovery and Long-Term Outlook
Recovery is slow but often steady. Many patients say the first sign of improvement is the ability to wiggle their toes or flex their ankles. Then comes sitting up, standing with help, and eventually walking with a cane. Pain and fatigue linger for months. Physical therapy, occupational therapy, and psychological support are critical.
There’s no cure for GBS yet, but with early IVIG, most people get back to their daily lives. The key is recognizing the signs early and acting fast. If weakness starts in the feet and climbs upward, don’t wait. Get to the hospital. Time is nerve.
Can Guillain-Barré Syndrome come back?
Most people have only one episode of GBS. Recurrence is rare-about 3% to 5% of patients experience a second episode. When it does happen, it’s usually years later and often less severe. Doctors monitor patients for any return of symptoms, especially if they’ve had recent infections or vaccinations.
Is IVIG safe for children with GBS?
Yes. IVIG is approved and commonly used in children with GBS. Dosing is adjusted by weight, and side effects are similar to adults: headaches, fever, and mild allergic reactions. Children often recover faster than adults, and IVIG significantly reduces hospital stay and time to walking. Pediatric neurologists follow the same guidelines as for adults, with close monitoring for kidney function and blood pressure.
Why does IVIG cause headaches?
The exact reason isn’t fully understood, but it’s likely due to a temporary increase in pressure inside the skull or an immune response to proteins in the immunoglobulin. Headaches usually start during or shortly after the infusion and can be severe. Doctors often give pain relievers like acetaminophen before or during treatment. Staying well-hydrated can also help reduce this side effect.
Can you get GBS from a vaccine?
Very rarely. The risk is estimated at about 1 to 2 cases per million doses. The most studied link is with the 1976 swine flu vaccine, which had a slightly higher incidence. Modern vaccines, including flu and COVID-19 shots, show no significant increase in GBS risk. The benefits of vaccination far outweigh this tiny risk. In fact, infections like the flu or COVID-19 themselves are much more likely to trigger GBS than vaccines.
How long does IVIG stay in your system?
The infused antibodies from IVIG last about 3 to 4 weeks in the bloodstream. That’s why a 5-day course is given-to maintain effective levels during the critical phase of nerve damage. The treatment doesn’t cure GBS; it helps the immune system reset. After that, the body slowly clears the antibodies, and recovery depends on the nerves healing on their own.
Nishan Basnet
March 21, 2026 AT 17:09Just wanted to say thank you for laying this out so clearly. I’ve seen friends go through GBS, and the fear is real - that slow creep of weakness, the hospital monitors, the helplessness. IVIG felt like a lifeline, even with the headaches. One buddy said the first time he wiggled his toe after two weeks, he cried. It’s not glamorous, but it’s human. And honestly? That’s what matters.
Desiree LaPointe
March 22, 2026 AT 14:59Oh honey, let me guess - you’re one of those people who thinks IVIG is ‘magic fairy dust’ because some JAMA study says so? Let’s not ignore that 20% of patients still end up in wheelchairs while the pharmaceutical industry rakes in $20K per bag. And don’t get me started on how ‘safe’ it is - kidney failure? Really? That’s not a side effect, that’s a feature of the healthcare industrial complex. Wake up.
trudale hampton
March 23, 2026 AT 16:14My cousin went through this last year. IVIG was rough - she said the headaches felt like someone was tightening a steel band around her skull - but she walked out of rehab six months later with just a slight limp. The nurses told her the fact that she started treatment within 48 hours made all the difference. It’s scary, but there’s hope. Keep pushing through the pain. You’re not alone.
Paul Cuccurullo
March 24, 2026 AT 05:02It’s astonishing how much we’ve advanced in understanding immune-mediated neuropathies, yet so many still treat GBS as a mysterious, almost mythical affliction. The data is unequivocal: early IVIG intervention correlates directly with improved functional outcomes. The emotional weight of this condition cannot be overstated - but neither can the scientific rigor behind its treatment. We must not let anecdote override evidence.
Solomon Kindie
March 25, 2026 AT 17:33Natali Shevchenko
March 27, 2026 AT 15:38I’ve been thinking about this a lot lately - not just as a patient advocate, but as someone who’s watched time slip through fingers in a hospital room. IVIG doesn’t heal nerves. It buys time. It’s a pause button on the immune system’s rampage. What really heals is the slow, silent work of axons regrowing, of synapses rekindling, of muscles remembering how to fire. We celebrate the drug, but the body - the quiet, stubborn, miraculous body - is the real miracle. And it needs patience. Not just medicine.
Chris Dwyer
March 28, 2026 AT 15:48Just want to say - if you or someone you love is going through this, you’re doing better than you think. Recovery isn’t linear. Some days you’ll feel like you’re backsliding. That’s normal. Celebrate the tiny wins: lifting a spoon, standing for 10 seconds, wiggling a toe. You’re not broken. You’re rebuilding. And you’ve got a whole community behind you. Keep going. One step at a time.
shannon kozee
March 30, 2026 AT 10:13IVIG isn’t perfect, but it’s the best tool we have right now. Early treatment saves function. That’s the bottom line.